As the nation struggles with the most pervasive health crisis for one hundred years, the central role of hospitals as community resources for all, irrespective of residence, nationality or ethnic background, is obvious. Today we would expect patients to be treated solely on medical need. Yet in the interwar period, an era of significant expansion in hospital infrastructures, such issues of belonging and exclusion dominated the discourse and policy that framed institutional development.
The 1930s saw extensive plans for hospital building across Europe, North America and Australasia as institutional care expanded and patient numbers grew. In Britain, rationalised developments that brought together a number of providers on one site, often in a suburban area, were mooted for places like Middlesbrough, Aberdeen and Bristol. In Birmingham, the new Queen Elizabeth Hospital, funded entirely by philanthropic donations, opened in 1939 on a green field site next to the University.

In Paris, on the other hand, Hôpital Beaujon in the northern suburb of Clichy was developed by Assistance Publique as a municipal resource. And in Hungary a rash of new builds sprang up along the country’s much reduced borders. Designed to compensate for hospitals lost to neighbouring nations, they were nationalist symbols, often named after political heroes. These creations highlight important themes about space, place and belonging which played out across the 1930s in major developments in Lille, Sheffield and Prague.
In 1932, the mayor of Lille, Roger Salengro, announced that he had commissioned the French American architect, Paul Nelson, to design a massive new hospital complex on a 60 acre site on the edge of the city (figure 1, banner image). The new Cité Hospitalière would merge three existing institutions and enhance them with a medical school, maternity unit, tuberculosis sanatorium and anti-cancer unit. But it was also going to be path-breaking in its design, with two 25 storey sky-scraper blocks – one in the shape of a cross, the other an open book. The venture would service the whole region, and the council applied to central government for loans to help meet the project’s 400 million franc price tag.
The plan provoked an outraged response from local politicians, the right-wing press and the architectural profession, who condemned the cost, the lack of transparency in the commissioning of the architect, and the ‘un-French’ design. This controversy revealed that new modernist projects like this were sites for a battle over national identity and culture in an increasingly insular and xenophobic world. Use of the Skyscraper was attacked as foreign, while Depeche complained that ‘for a construction of such importance, it would seem to us that there should have been a competition and with a preference given to a French architect’. The press got their way and Nelson’s plan was abandoned. In the subsequent competition the commission was won by Jean Walter, one of the architects of Beaujon who adapted a number of the themes of the Nelson design but on a smaller, more ‘European’ scale.

Million Pound Appeal launch brochure.
Issues of belonging, boundaries and entitlement were also raised by the proposal to unify voluntary hospital services for the northern English city of Sheffield in the second half of the 1930s. Soon after the First World War the philanthropically funded, voluntary hospitals in the city joined together to form the Sheffield Hospital Council and to launch a mutual insurance initiative – the Penny in the Pound scheme. Initially the Council was a loose collaboration but from the early 1930s a combination of financial pressure and inadequate hospital infrastructure pushed plans to merge the management of the institutions and to build a joint hospital.
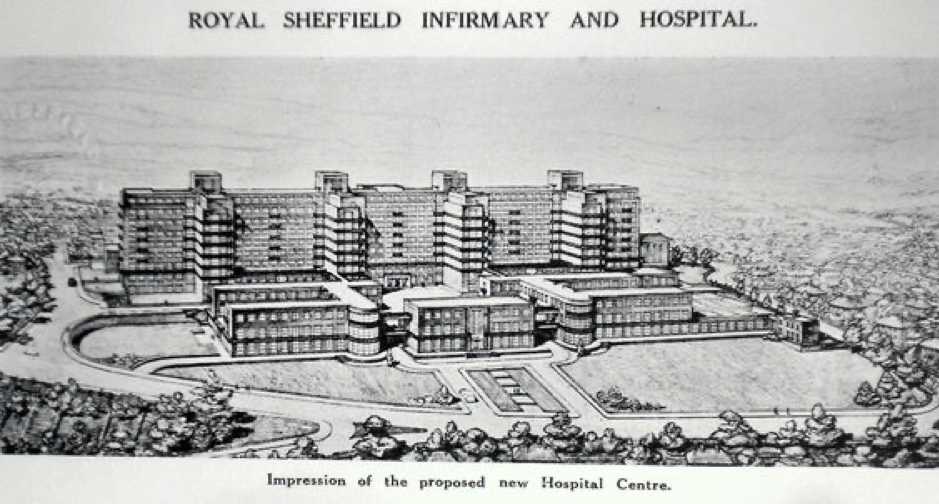
In 1938 a scheme was launched under the title The Shape of Things to Come to build a new single site hospital for acute general and specialist services; an extension to the city’s poor maternity provision; and a regional radium centre. Within a year a competition was held for a design for the new hospital won by Adams, Holden, Pearson. The new site was to be funded by the Sheffield Million Pound Appeal with responsibility for the target allocated to three groups – private subscribers, local businesses and workers. The Private subscribers would carry on the work of the traditional philanthropists. Firms would pledge £50k a year while 250,000 workers enrolled in a League of Hospital Builders would add a penny a week to their contributory insurance subscription. But the role of the local state was limited, with municipal authorities targeted as potential donors but not as part of the hospital’s planning.
Tension between the voluntary and municipal sectors grew as a result, especially after the new hospital plan was unveiled without consultation with the council. This snub, and the plan to relegate the municipal providers to an ancillary role, infuriated the Labour council. They felt the voluntary hospital plans would not meet the needs of the people of Sheffield. The new hospital would be regional and specialist rather than Sheffield focused, with the effect that the local authority would be supporting a project that did not benefit its own citizens. Council services were handicapped by legal requirements that limited the geographical area from which they could take patients. It was therefore difficult for them to develop their own specialist services while the voluntary sector continued to expand. Furthermore, the development relied on much of the routine hospital work – such as road and work place accidents and caring for long stay and ‘chronic’ cases – being picked up by the municipal provision.
The Royal Infirmary, Sheffield, Annual Report 1940
In the end the Labour Party led council refused to give their blessing – or any money – to the new developments and instead launched a raft of competing projects, including a 600 bed general hospital for medical and surgical cases and a modern sanatorium of 420 pulmonary TB beds. Both schemes, however, were held up by the war, and then ultimately abandoned by the newly formed NHS in 1948.
Our third example explores nation and belonging in the tense Czech-German politics of late 1930s Prague. German speakers accounted for over twenty percent of the Czechoslovak population, the vast majority living in the province of Bohemia. In interwar Czechoslovakia, they maintained a prominent role in health provision and as a result both Czech and German speaking doctors were trained and practised in Prague’s main hospital, alternating clinics on a weekly basis. As the Czechs gradually came to dominate Charles University, the Germans formed their own German University and Medical School. They guarded these medical facilities jealously, leading to significant duplication of services, and some tension. For example, in the late 1930s a Rockefeller Foundation nurse training centre in Prague collapsed in disarray when the German student refused to be taught with their Czech compatriots.

By the late 1930s it was agreed that a new hospital and medical school were needed in Prague city centre. The scheme was approved by Parliament, and in 1938 plans were drawn up by a group of leading Czech medics. In their scheme two separate buildings were envisaged with a 2,800 bed Czech institution and a 1,200 bed German facility on the same site. Although it was recognised that they should share key services like catering, laundry and laboratories, all medical facilities were to be duplicated across the two institutions, including separate admissions and outpatient departments.
The present Coronavirus crisis has seen the health services of England, Scotland and Wales commission vast temporary hospitals in exhibition centres in our major cities. These centrally located facilities will undoubtedly seek to serve the whole community irrespective of locality, ethnicity or nationality. In the interwar world of scarce resources and extreme political views, however, hospitals had become sites of conflict over national interest versus municipal socialism; the citizens versus outsiders; and ethnic group versus ethnic group. In the process the boundaries defining who was and was not a suitable case for treatment solidified, excluding as well as including members of the hospital community.
Barry Doyle is Professor of Health History at the University of Huddersfield. He has worked extensively on the history of urban healthcare, with a particular focus on pre-NHS provision, detailed in his monograph The Politics of Hospital Provision in Early Twentieth-Century Britain (Routledge, 2014). He is currently working with Dr Rosemary Cresswell on the AHRC-funded project ‘Crossing Boundaries: The History of First Aid in Britain and France, 1909-1989’ and completing a University of Huddersfield funded examination of hospital provision in Central Europe between the wars.
Figure 1. (Banner Image). Model of Paul Nelson’s planned hospital complex for Lille, 1932. Archives Municipales de Lille, Suite des travaux et inauguration : coupures de presse. 3M/1/19
Figure 2. Dépêche: ‘Petite Chronique Local de la Semaine’ 7 Jan 1933. Archives Municipales de Lille, Suite des travaux et inauguration : coupures de presse. 3M/1/19
Figure 3. Front cover for the Sheffield Hospital Council’s Million Pound Appeal launch brochure. TNA MH58/319
Figure 4. Architect’s impression of new hospital Sheffield. The Royal Infirmary, Sheffield, Annual Report 1940
Figure 5. Plan for new Hospital and Medical School, Prague, 1937. Source: Havlicek, Uklein, Albert, ‘Study of A Health Centre and University Medical School at Prague’, Nosokomeion, (1938), 210.
Due to their age, all images are understood to be free of copyright restrictions.

Leave a comment